Elucidation of periostin related to the onset of itch in atopic dermatitis and discovery of its therapeutic agent
Atopic dermatitis (AD) is a chronic relapsing skin disease accompanied by recurrent itching. Although type 2 inflammation is dominant in allergic skin inflammation, it is not fully understood how non-type 2 inflammation co-exists with type 2 inflammation or how type 2 inflammation causes itching. We have recently established a mouse model of AD. named facial atopic dermatitis with scratching (FADS) mouse by selectively deleted IKK2, a positive regulator for the NF-κB signaling. FADS mice exhibit eczema lesions limited to the face, probably because of the expression of nestin in facial dermal fibroblasts derived from neural crest cell. (J. Invest. Dermatol. 139, 1274, 2019, J Allergy Clin. Immunol. 148, 1596, 2021)
Periostin, a downstream molecule of type 2 inflammation plays a critical role in the pathogenesis of allergic skin inflammation. We have previously demonstrated the fibroblasts are the main periostin producing cells in AD skin lesions (J. Clin. Invest 122, 2590, 2012). To elucidate the functional roles of periostin in the onset or progression of skin inflammation in FADS mice, we applied a genetic approach to disrupt periostin by generating FADS/PostinLacZ/LacZ mice. Periostin deficiency did not prevent the onset of facial eczema; it appeared around postnatal day 10; it also did the control mice. However, eczema did not develop thereafter, and the eczema was significantly improved with compared with FADS/Postin+/+ mice at both P17 and P28 in FADS/PostinLacZ/LacZ mice. (Figure 1)
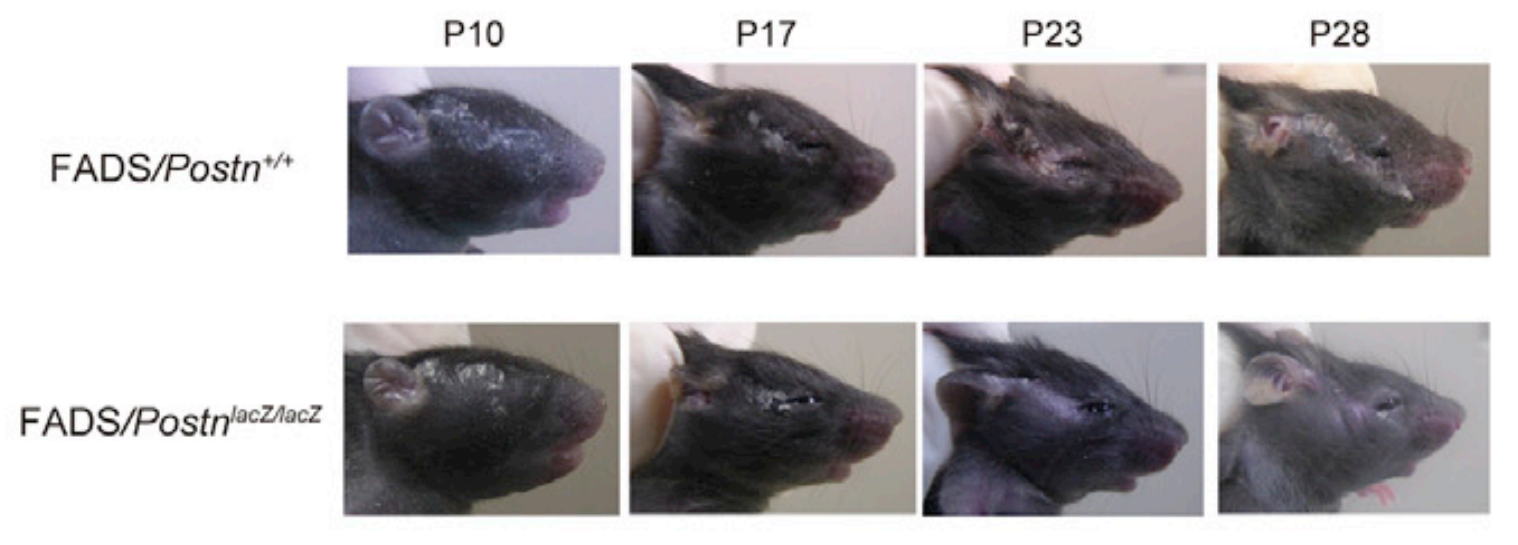
Fig 1. Macroscopic facial skin lesions of FADS/PostinLacZ/LacZ mice and FADS/Postin+/+ mice at the indicated periods after birth.
In FADS mice, inhibition of periostin by genetic disruption inhibits NF-κB activation in keratinocytes, leading to downregulating eczema, epidermal hyperplasia, and infiltration of neutrophils, without regulating the enhanced type 2 inflammation. Moreover, inhibition of periostin blocks spontaneous firing of superficial dorsal horn neurons followed by a decrease in scratching behaviors due to itching.
We have previously shown that CP4715, an αvβ3 integrin inhibitor, potently inhibits the binding of periostin to the receptor (Am. J. Respir. Cell Mol. Biol.62,204,2020). We examined the effects of CP4715 administration into FADS mice on skin inflammation and itching. Continuous administration of CP4715 improved eczema, epidermal thickness and infiltration of neutrophils, mast cells and M2 macrophages.
We next examined the effects of single shot administration of CP4715 on itching and spontaneous firing of neurons in FADS mice. The single shot immediately started to decrease the spontaneous firing of neurons, its inhibitory effect reaching the maximum at 40 min after administration (Fig 2). Scratching bouts were immediately decrease after 40 min as well, indicating that the effects of periostin on sensoryneuron cells are probably direct.
Taken together, periostin links NF-κB-mediated inflammation with type 2 inflammation and promotes itching in allergic skin inflammation, suggesting that periostin is a promising therapeutic target for AD.
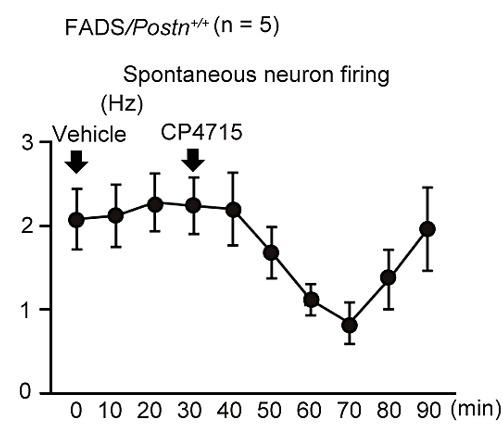
Fig. 2. Effects of spontaneous firing of dorsal horn neurons by CP4715.
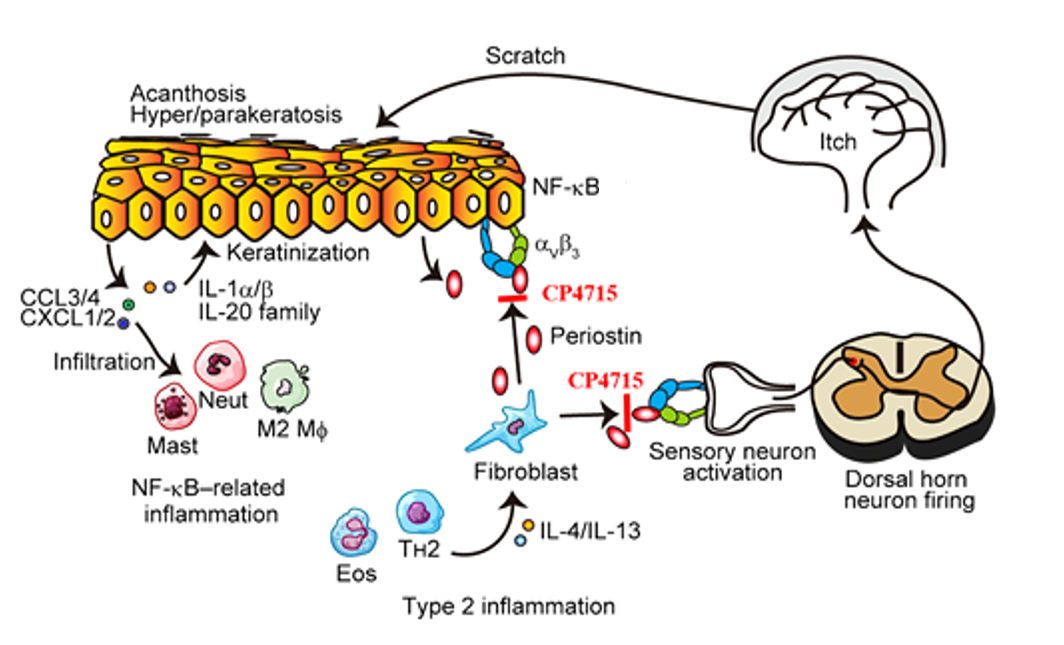
Graphical abstract
- Periostin links NF-kB-related inflammation with type 2 inflammation.
- Periostin drives the spontaneous firing of dorsal horn neurons related with itching.
- Pharmacological blockage of periostin (CP4715) suppresses skin inflammation and itching.
Original article information
Journal
Cell Reports 42,11193, January 31, 2023
Title
Periostin activates distinct modules of inflammation and itching downstream of the type 2 inflammation pathway.
Authors
Satoshi Nunomura, Daisuke Uta, Isao Kitajima, Yasuhiro Nanri, Kosuke Matsuda, Naoko Ejiri, Midori Kitajima, Hitoshi Ikemitsu, Misaki Koga, Sayaka Yamamoto, Yuko Honda, Hironobu Takedomi, Tsugunobu Andoh, Simon J. Conway, Kenji Izuhara

